You’re standing in the pharmacy aisle staring at a wall of creams, gels, and rubs — all claiming to fight inflammation and pain. Some contain diclofenac. Others list menthol, capsaicin, or arnica. A few just say “fast-acting relief.” None of them explain which one actually matches what you’re dealing with.
Anti-inflammatory creams are topical formulations designed to reduce inflammation, pain, and swelling at the site of application. They range from over-the-counter (OTC) options available without a prescription to prescription-strength formulations requiring medical authorization. Choosing the wrong type doesn’t just waste money — it can delay real relief or cause unnecessary side effects.
This guide covers every major category of anti-inflammatory cream, how each one works, which conditions each is best suited for, and what to watch out for. It also includes a condition-to-ingredient matching table and a comparative safety overview — two things most guides in this space simply don’t provide.
This guide is for adults managing joint pain, muscle inflammation, arthritis, or inflammatory skin conditions who want to make an informed, evidence-based choice.
Table of Contents
Key Takeaways
- What are anti-inflammatory creams? → Topical products that reduce pain and inflammation at the application site without requiring oral medication.
- Best for joint/muscle pain? → Topical NSAIDs (diclofenac) are the most evidence-backed OTC option.
- Best for skin inflammation? → Corticosteroid creams (hydrocortisone OTC; stronger versions by prescription).
- OTC vs. prescription? → Diclofenac 1% (Voltaren) is now available OTC; high-potency corticosteroids and most other NSAIDs require a prescription.
- Biggest mistake? → Using a counterirritant cream (menthol, methyl salicylate) for a condition that needs a true anti-inflammatory — they work completely differently.
What Are Anti-Inflammatory Creams?
Anti-inflammatory creams are topical preparations that deliver active ingredients through the skin to reduce localized inflammation. They work by inhibiting specific biological pathways — primarily the COX enzyme pathway (for NSAIDs) or the immune response cascade (for corticosteroids) — at the site of application rather than systemically throughout the body.
This localized delivery is the key clinical advantage. According to research summarized by the U.S. National Library of Medicine, topical diclofenac produces measurable therapeutic concentrations in underlying joint tissue while keeping systemic blood levels significantly lower than equivalent oral doses — meaningfully reducing the risk of gastrointestinal and cardiovascular side effects associated with oral NSAIDs.
How Absorption Actually Works
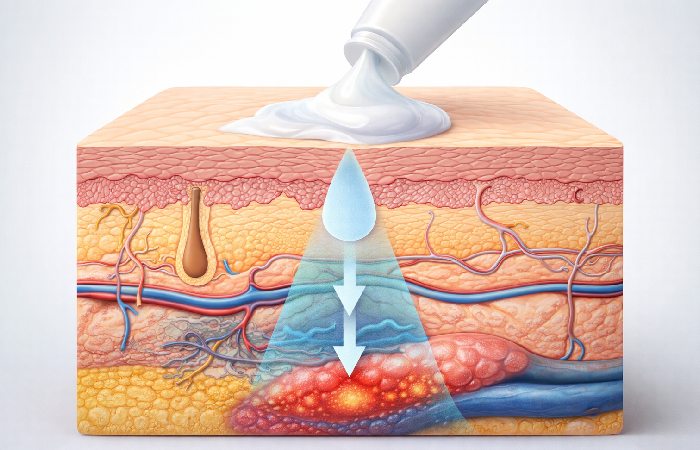
Here’s where most guides stop short. Getting an active ingredient from a cream into your joint or muscle requires it to penetrate the stratum corneum — the lipid-rich outermost skin layer that evolved to keep substances out.
Formulation matters far more than most consumers realize. Gel vehicles tend to penetrate inflamed tissue more effectively than thick cream bases. Penetration enhancers like ethanol are used in pharmaceutical formulations to improve delivery. Concentration, skin condition, application site, and how thoroughly you massage the product in all affect how much active ingredient actually reaches target tissue.
Types of Anti-Inflammatory Creams: A Full Breakdown
Not all “anti-inflammatory” creams work the same way. The label rarely makes this clear. Here’s what each category actually does — and what it doesn’t.
Topical NSAIDs
Topical non-steroidal anti-inflammatory drugs are the most clinically evidence-backed category for joint and musculoskeletal pain. They inhibit cyclooxygenase (COX-1 and COX-2) enzymes, which reduces the production of prostaglandins — the chemical mediators responsible for pain, heat, and swelling.
Key examples:
- Diclofenac sodium 1% gel (Voltaren Arthritis Pain) — OTC; FDA-approved for osteoarthritis of joints amenable to topical treatment
- Diclofenac sodium 1.5% solution — Prescription in some formulations
- Ibuprofen gel — Available OTC in the UK and EU; limited OTC availability in North America
- Ketoprofen gel — Prescription in most markets
Best for: Osteoarthritis (knees, hands, feet, elbows), tendinitis, minor joint inflammation
Key limitation: Evidence is strongest for osteoarthritis. For deep-tissue inflammation (hip joints), penetration to the target site may be insufficient for meaningful effect.
Corticosteroid Creams
Corticosteroids suppress the immune response that drives inflammatory skin conditions. They don’t work like topical NSAIDs — their mechanism is not primarily pain relief but inflammation suppression at the skin level.
Key examples:
- Hydrocortisone 0.5%–1% — OTC; lowest potency class; suitable for mild eczema, contact dermatitis, insect bites
- Betamethasone valerate 0.1% — Prescription; mid-to-high potency; for moderate-to-severe eczema and psoriasis
- Clobetasol propionate 0.05% — Prescription; highest potency class; for severe psoriasis and resistant dermatitis
- Triamcinolone acetonide — Prescription; mid-potency; broad dermatological use
Best for: Eczema, contact dermatitis, psoriasis, seborrheic dermatitis, allergic skin reactions
Key limitation: Not appropriate for joint pain, muscle pain, or musculoskeletal inflammation. These are skin-layer agents only — applying them to a sore knee will not reduce joint inflammation.
Capsaicin Creams
Capsaicin — the compound that makes chili peppers hot — works through an entirely different mechanism. It depletes substance P, a neuropeptide that transmits pain signals from peripheral nerves to the central nervous system. With repeated application, nerve endings become desensitized and the pain signal diminishes.
Key examples:
- Capsaicin 0.025%–0.1% cream — OTC; standard formulation for osteoarthritis and neuropathic pain
- Capsaicin 8% patch (Qutenza) — Prescription only; single application in clinical settings for severe neuropathic pain
Best for: Osteoarthritis, neuropathic pain (diabetic neuropathy, post-herpetic neuralgia), chronic musculoskeletal pain
Key limitation: Causes a significant burning sensation on initial use — typically for the first 2–4 weeks. That sensation is the mechanism working, not a side effect to be alarmed by. Not suitable for broken or actively inflamed skin.
Counterirritants (Menthol, Methyl Salicylate, Camphor)
This is the category that most guides get wrong — by not distinguishing it clearly enough from true anti-inflammatories.
Counterirritants create a competing sensation (warmth from methyl salicylate, cooling from menthol) that temporarily overrides pain perception via the gate-control mechanism. They do not meaningfully inhibit prostaglandins or suppress immune activity. Relying on them for an inflammatory condition that needs a pharmaceutical response is a common and costly mistake.
Key examples:
- Methyl salicylate — Found in many topical pain products
- Menthol creams (Biofreeze, Bengay, IcyHot) — Cooling sensation via TRPM8 receptor activation
- Trolamine salicylate — Mild topical analgesic
Best for: Temporary symptomatic relief of muscle aches, minor sports injuries, sore muscles
Not for: Chronic inflammatory conditions, arthritis, skin inflammation
Natural and Herbal Options
Natural anti-inflammatory creams span a wide spectrum of evidence quality. Some have reasonable clinical support; others remain largely anecdotal.
Key examples:
- Arnica montana — Some evidence for reducing bruising, post-surgical swelling, and muscle soreness; mechanism not fully established
- Turmeric/curcumin — Topical curcumin has demonstrated anti-inflammatory properties in lab settings; human clinical trial evidence for topical use in joints remains early-stage
- CBD (cannabidiol) — Anti-inflammatory properties documented in preclinical research; large-scale human trials for topical use are still limited
- Calendula — Used for minor skin inflammation; primarily soothing rather than deeply anti-inflammatory
Best for: Minor bruising, muscle soreness, skin redness, those preferring non-pharmaceutical formulations
Key limitation: Evidence is substantially weaker than pharmaceutical options. Natural options are appropriate for mild, self-limiting conditions — not as the primary treatment for diagnosed inflammatory disease.
Condition-to-Ingredient Matching Table
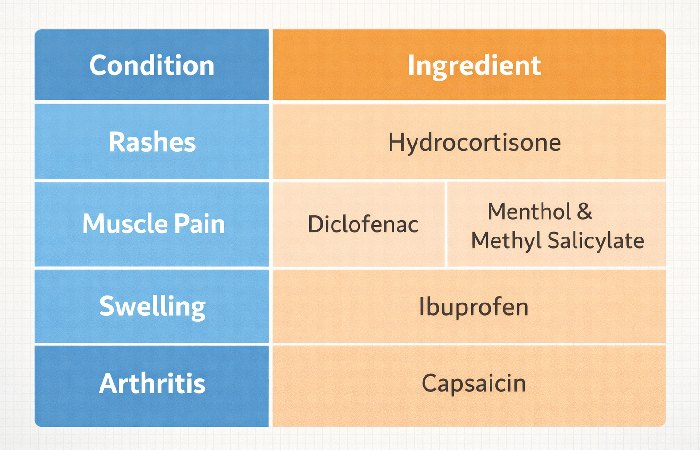
Most guides list ingredient categories but leave readers to figure out the match themselves. This table does the work for you.
| Condition | First-Line Topical Option | Second-Line Option | Avoid |
|---|---|---|---|
| Osteoarthritis (knee, hand, elbow) | Topical NSAID (diclofenac) | Capsaicin cream | Corticosteroids; counterirritants as primary treatment |
| Muscle soreness / sports injury | Menthol/methyl salicylate (symptomatic) | Topical NSAID | Corticosteroids |
| Eczema / contact dermatitis | Hydrocortisone (OTC) or Rx corticosteroid | Barrier cream | Capsaicin, NSAIDs |
| Psoriasis | Prescription corticosteroid | Coal tar preparations | Capsaicin on active plaques |
| Tendinitis | Topical NSAID (diclofenac) | Ice + rest | Unsupervised corticosteroids |
| Neuropathic pain (chronic) | Capsaicin 0.025%–0.1% | Topical lidocaine | Standard counterirritants |
| Minor bruising | Arnica gel | None typically required | High-potency corticosteroids |
| Back pain (muscle origin) | Menthol/counterirritant (symptomatic) | Topical NSAID | Corticosteroids |
OTC vs. Prescription: How to Know Which You Need
The OTC vs. prescription distinction matters both practically (access, cost) and clinically (potency, safety monitoring requirements).
What’s Available Over the Counter
- Diclofenac sodium 1% gel — The most significant recent OTC change in this category. FDA-approved for osteoarthritis, available as Voltaren Arthritis Pain in the US and equivalent products internationally.
- Hydrocortisone 0.5%–1% — Available OTC for mild skin inflammation; short-term use only.
- Capsaicin up to 0.1% — OTC in standard low-dose formulations.
- Counterirritants — All menthol, methyl salicylate, and camphor-based products are OTC.
What Requires a Prescription
- Higher-concentration diclofenac formulations (certain solutions and gels)
- Mid-to-high potency corticosteroids (betamethasone, clobetasol, triamcinolone) — require physician oversight due to skin thinning and hormonal suppression risks with extended use
- Capsaicin 8% patch (Qutenza) — prescription only, applied in clinical settings
- Ketoprofen and flurbiprofen gels — prescription in most markets
As the U.S. Food and Drug Administration explains, OTC classification requires that a product can be used safely and effectively without professional supervision — which is precisely why higher-potency formulations remain prescription-gated.
Comparative Safety Profiles
Every ingredient category carries a different risk profile. This is the side-by-side comparison most consumer guides leave out.
| Ingredient Type | Key Risks | Long-Term Use Guidance | Drug Interactions |
|---|---|---|---|
| Topical NSAIDs | Skin irritation, photosensitivity; low systemic absorption | Generally acceptable for weeks to months with physician guidance | Caution with oral NSAIDs (NSAID doubling); caution with oral anticoagulants (warfarin) |
| OTC Corticosteroids | Skin thinning, pigmentation changes with prolonged use | OTC hydrocortisone: max 7 days per label; avoid face/groin without guidance | Minimal systemic interactions at OTC doses |
| Prescription Corticosteroids | HPA axis suppression, skin atrophy, striae, increased infection risk | Must be physician-managed; not suitable for indefinite use | Potential for systemic corticosteroid interactions at high doses over large areas |
| Capsaicin | Burning sensation (especially first 2 weeks); avoid mucous membranes | Low systemic risk; generally safe for ongoing use | Minimal drug interactions |
| Counterirritants | Skin irritation; methyl salicylate is absorbed and can be toxic if applied in large amounts under occlusive dressings | Safe for periodic use | Methyl salicylate: caution with warfarin |
| Natural/Herbal | Allergic reactions possible; variable quality control | Low systemic risk for most options | CBD: potential interactions with anticoagulants and some statins |
Critical note on drug interactions: Topical NSAIDs combined with oral NSAIDs (ibuprofen, naproxen, aspirin) push total NSAID exposure above safe thresholds. If you’re taking oral NSAIDs regularly, discuss topical NSAID use with your pharmacist before adding a cream to your routine. This interaction is real and consistently underestimated in consumer-facing content.
How to Use Anti-Inflammatory Creams Correctly
Application method affects both efficacy and safety. These aren’t just label formalities.
- Clean the skin — Wash and dry the application area first. Dirt and surface oils can reduce absorption and increase irritation risk.
- Apply the correct amount — More is not better. Diclofenac gel, for instance, is dosed by the packet (typically 2g per small joint, 4 times daily for Voltaren). Excess application increases systemic absorption without improving local concentration.
- Rub in thoroughly — Massage gently until absorbed. For joint areas, apply around the joint, not just over the central skin surface.
- Wash hands after — Unless treating the hands. Avoid touching eyes, mouth, or mucous membranes after application.
- Avoid occlusive dressings (unless directed) — Wrapping the area significantly increases absorption. For counterirritants, this can reach toxic levels of methyl salicylate.
- Wait before heat or water exposure — Avoid heating pads immediately after applying any cream and wait at least 60 minutes before bathing or swimming.
Frequency: Follow product label instructions exactly. Topical NSAIDs are typically 3–4 times daily. OTC hydrocortisone: up to 3–4 times daily, maximum 7 days without medical guidance. Capsaicin requires 3–4 applications daily minimum — the substance P depletion mechanism demands consistency. Skipping days resets the clock.
Common Mistakes to Avoid
- Treating a counterirritant as an anti-inflammatory — Menthol and methyl salicylate create a sensation. They do not reduce prostaglandins or suppress immune response. If you need genuine inflammation control, these products won’t deliver it.
- Applying corticosteroid cream to large areas or the face without guidance — Even OTC hydrocortisone carries risks with widespread or prolonged use: skin thinning, pigmentation disruption, and — with high-potency Rx steroids — systemic hormonal effects.
- NSAID doubling — Taking oral ibuprofen or naproxen while applying diclofenac gel means two NSAIDs simultaneously. This isn’t automatically forbidden, but it increases the load on your kidneys, liver, and gastrointestinal tract. Tell your pharmacist.
- Quitting capsaicin after a few days due to burning — The burning is the mechanism. Substance P depletion takes 2–4 weeks of consistent use. Most people abandon it during the window when it’s actually starting to work.
- Expecting topical creams to replace systemic treatment for deep-joint or severe disease — Topical formulations are most effective for superficial joints (hands, knees, elbows). For hip arthritis or systemic inflammatory disease, oral or injectable treatment is typically still necessary.
- Applying near open wounds or broken skin — Active ingredients penetrate broken skin dramatically faster, increasing both risk and unpredictability of absorption.
Who Anti-Inflammatory Creams Are For — and When to See a Doctor
Best suited for:
- Adults managing mild-to-moderate osteoarthritis in accessible joints (hands, knees, elbows, wrists)
- Athletes and active adults with muscle soreness, minor strains, or tendinitis
- People dealing with mild-to-moderate inflammatory skin conditions (eczema, contact dermatitis)
- Adults who cannot tolerate oral NSAIDs due to GI sensitivity or kidney concerns
- Older adults (60+) managing osteoarthritis who want to minimize systemic medication exposure — topical diclofenac is particularly relevant here, as the Arthritis Foundation identifies it as a recommended option for older patients seeking to reduce gastrointestinal risk
See a doctor before or instead if:
- Pain or inflammation is severe, sudden, or worsening despite consistent topical treatment
- You’ve used OTC corticosteroids for more than 7 days without improvement
- You have rheumatoid arthritis or any autoimmune inflammatory condition — systemic treatment is typically required
- You’re taking anticoagulant medication (warfarin, rivaroxaban) — discuss the interaction risk before adding a topical NSAID
- You’re pregnant or breastfeeding — topical NSAIDs and high-potency corticosteroids have precautionary restrictions during pregnancy
- A skin condition spreads beyond the initial area or fails to respond to OTC treatment within 2 weeks
Final Verdict: How to Choose the Right Anti-Inflammatory Cream
The right anti-inflammatory cream isn’t the one with the most recognizable brand or the longest ingredient list. It’s the one that actually matches your condition.
Dealing with joint pain from osteoarthritis? Start with a topical NSAID like diclofenac. It’s the most evidence-backed OTC option available and is now accessible without a prescription in most markets. Managing an inflammatory skin condition like eczema or contact dermatitis? A corticosteroid cream — hydrocortisone for mild cases, a prescription formulation for anything moderate-to-severe — is the right tool. Temporary muscle soreness or a minor sports strain? A menthol or methyl salicylate product provides fast symptomatic relief without the need for pharmaceutical actives.
Natural options like arnica and CBD creams can support mild, self-limiting conditions — but they should not substitute for evidence-based treatment when a genuine inflammatory process needs addressing.
If you’re taking oral NSAIDs or any anticoagulant, flag your anti-inflammatory cream use to your pharmacist. The drug interaction risk is real, clinically relevant, and consistently underreported.
Frequently Asked Questions
Q: What is the strongest anti-inflammatory cream available over the counter?
A: Diclofenac sodium 1% gel (Voltaren Arthritis Pain) is the most clinically evidence-backed OTC anti-inflammatory cream for joint pain. For inflammatory skin conditions, 1% hydrocortisone is the strongest OTC corticosteroid available. “Strongest” depends entirely on the condition — the right match matters more than concentration alone.
Q: What is the difference between an anti-inflammatory cream and a pain relief cream?
A: An anti-inflammatory cream targets the biological cause of inflammation — reducing prostaglandins (NSAIDs) or suppressing immune activity (corticosteroids). A pain relief cream like menthol or a counterirritant creates a competing sensation that temporarily masks pain without addressing the underlying inflammatory process. Both reduce perceived pain, but only true anti-inflammatory formulations address the root cause.
Q: Can I use anti-inflammatory cream and take ibuprofen at the same time?
A: Combining topical diclofenac (a topical NSAID) with oral ibuprofen or naproxen means two NSAID sources running simultaneously. This increases the total NSAID load on your body and raises the risk of kidney, liver, and gastrointestinal effects. It is not automatically prohibited, but discuss concurrent use with your pharmacist, especially if oral NSAIDs are part of your regular routine.
Q: How long does it take for anti-inflammatory cream to work?
A: Topical NSAIDs like diclofenac typically produce noticeable pain relief within 1–3 days of consistent use. Capsaicin creams require 2–4 weeks before significant pain relief occurs — the substance P depletion mechanism takes time, and most people stop too early. Corticosteroid creams for skin conditions often show visible improvement within 3–7 days.
Q: Are anti-inflammatory creams safe for long-term use?
A: It depends entirely on the ingredient. Topical NSAIDs can be used for weeks to months with physician guidance. OTC hydrocortisone should not exceed 7 consecutive days on any area without medical guidance due to skin thinning risk. Prescription corticosteroids require physician-managed monitoring for extended use. Capsaicin and most natural options carry low systemic risk for ongoing use.
Q: Do anti-inflammatory creams actually penetrate deep enough to work?
A: For superficial joints — knees, fingers, elbows, wrists — the clinical evidence supports meaningful tissue penetration. Studies show diclofenac gel produces measurable concentrations in knee synovial tissue. For deep joints like the hip, topical penetration is generally insufficient on its own, and systemic options are typically needed alongside — or instead of — topical formulations.
About Marketingsguide
Marketingsguide.com publishes practical, easy-to-understand content on health, technology, business, marketing, and lifestyle. Articles are based mainly on reputable, publicly available information, with AI tools used only to help research, organise, and explain topics more clearly so the focus stays on real‑world usefulness rather than jargon or unnecessary complexity.
Disclaimer
This guide is for general information only and does not replace professional medical advice, diagnosis, or treatment. Always consult a qualified healthcare provider about your specific symptoms, medications, and treatment options, and never ignore or delay medical care because of something you read online.
